Move Forward for movement longevity
Your Next Race Is Around the Corner. Specializing in Hybrid Athlete Longevity in Tampa & St. Pete
Stop managing pain and start building true resilience. Together, let’s maximize your performance and ensure longevity, so you can train harder and move forward for life.
Experience Tampa’s Top-Rated Physical Therapy
See why Tampa athletes, runners, and fitness enthusiasts choose Forward Physio. Our South Tampa clinic offers performance-focused, one-on-one physical therapy that gets results.
Physical Therapy for People Who Actually Train.
You’ve probably been to PT before. Fifteen minutes with the doc, forty-five minutes doing clamshells with a tech, a sheet of exercises you could’ve Googled. That model doesn’t work for someone training 5–6 days a week. We built Forward Physio for athletes who need more than rehab — you need a program that keeps up with the way you train.
Built for hybrid athletes: lifters who run, runners who lift, and Hyrox.
- 100% One-on-One Sessions with Your Doctor
- Both Doctors are SFMA Level 1 & Dry Needling Certified
- Serving Tampa Bay’s Bodybuilders, Runners & Weekend Warriors
- Direct Access – No Referral Needed in Florida
- Barbell rehab certified


Treatment That Moves Tampa Bay Forward
Whether you’re joining a run club, getting read for Hyrox, or preparing for your next competition, we help active Tampa and St. Petersburg residents reach peak performance. Dr. Tanner and Dr. Xu specialize in treating hybrid athletes who love to lift, run, and challenge their limits.

3 Steps to Functioning Forward
- Clarity first
- Strength second
- A return to training and living that is powerful, not cautious
We clarify the “why” behind your limitations and create a tailored plan that rebuilds your foundation, improves your strength and stability, and helps you return to performing with confidence instead of hesitation.
PT Tips for Tampa Athletes

Plantar Fasciitis in Tampa: A Runner’s Guide to Diagnosis, Loading, and the Real Fix
A doctor-led guide to plantar fasciitis for Tampa runners – what’s actually going on in the heel, how to keep training through it, and the loading protocol that fixes it…
Continue Reading…
Physical Therapy for Runners in Tampa: A Doctor-Led Guide
The five injuries we see most in Tampa Bay runners, why insurance-driven PT keeps failing them, and how one-on-one performance PT actually gets runners back on the road…
Continue Reading…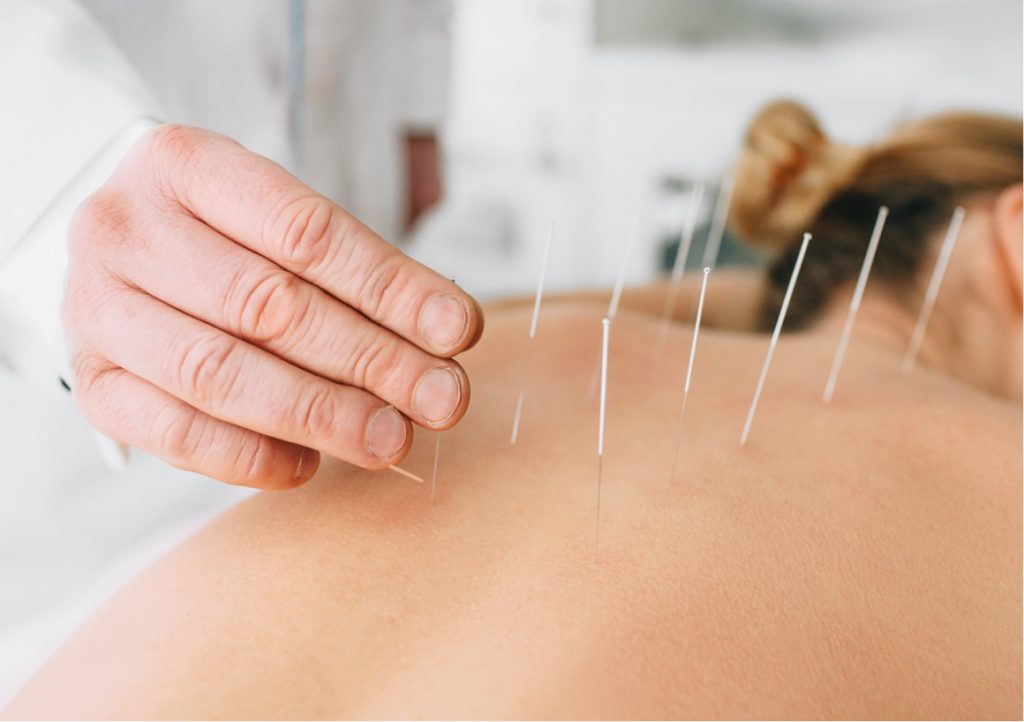
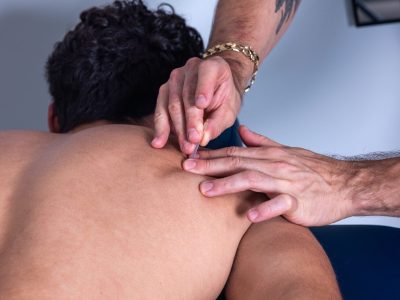
Dry Needling in Tampa: A Performance PT’s Guide for Runners, Lifters, and Hybrid Athletes
What dry needling actually is, how it works on athletic tissue, who it helps in Tampa Bay, and what a one-on-one session at Forward Physio looks like…
Continue Reading…